Hospital data has grown faster than the systems built to manage it. EHRs, imaging archives, claims feeds, and real-time operational workflows now generate volumes that legacy BI platforms (Cognos, SSRS, SAP BO, Qlik) were never designed to handle. The gap is no longer a future problem. It is showing up today in slow reports, compliance gaps, and clinical teams making decisions without current data.
At the same time, HIPAA, HITECH, and GDPR requirements have raised the bar for how patient health information must be stored, accessed, and audited. Modern cloud-native platforms meet those requirements by design. Legacy tools require costly workarounds that still leave gaps.
In this article, we’ll cover why healthcare organizations are accelerating BI migration, what modern architecture looks like, which platforms lead the category, a 9-step migration roadmap, proven best practices, real-world outcomes, and what the next generation of healthcare BI will require.
Key Learnings
- Modern BI migration is essential for healthcare due to rising data volumes from EHRs, imaging systems, telemedicine, and operational workflows.
- Cloud-native platforms like Fabric, Databricks, and Snowflake offer the scalability, compliance, and real-time processing legacy BI tools cannot provide.
- A strong migration strategy must prioritize HIPAA/HITECH security, PHI protection, semantic consistency, and robust governance.
- High-value dashboards such as patient flow, infection control, and readmission analytics deliver quick wins and support clinical operations.
- Future BI will integrate AI, LLM copilots, real-time hospital analytics, and multi-cloud architectures to enable proactive, data-driven healthcare.
Elevate Your Enterprise Reporting by Migrating to Power BI!
Partner with Kanerika for Expert Migration Services
Why Healthcare Enterprises Need BI Migration
Healthcare generates more data per organization than almost any other industry, and the rate is accelerating. Electronic health records alone now produce clinical, operational, and administrative data at a pace that most hospital reporting infrastructure, built a decade ago, was not designed to process.
The downstream effects are measurable. According to the U.S. Department of Health and Human Services, healthcare data volumes have grown by over 30% annually across major systems since 2020. HIMSS research further shows that data complexity now ranks among the top three barriers health systems cite when evaluating analytics modernization. Legacy platforms that took hours to run a patient census report now struggle with queries that modern cloud warehouses execute in seconds. KLAS Research’s Data & Analytics Platforms 2025 report similarly found that turning data into actionable insights remains a significant challenge for most health systems, with proactive vendor support – not platform features alone – determining whether analytics investments deliver real outcomes.
The compliance dimension makes this more urgent. HIPAA and HITECH require audit logging, access controls, and data lineage tracking at a level that most on-premise BI deployments cannot enforce without significant custom development. The HHS HIPAA Security Rule mandates technical safeguards that modern cloud platforms implement natively. GDPR adds requirements for any healthcare organization managing data for European patients.
Beyond compliance, the clinical demand has shifted. Infection control teams, population health managers, and hospital operations leaders now need real-time dashboards, not the static reports refreshed overnight that batch-processing tools deliver. Legacy tools built for batch processing cannot meet that requirement without architectural changes that cost as much as a full migration. Proper data governance must be in place before any of that real-time access is safe to enable.
Modern BI Architecture for Healthcare
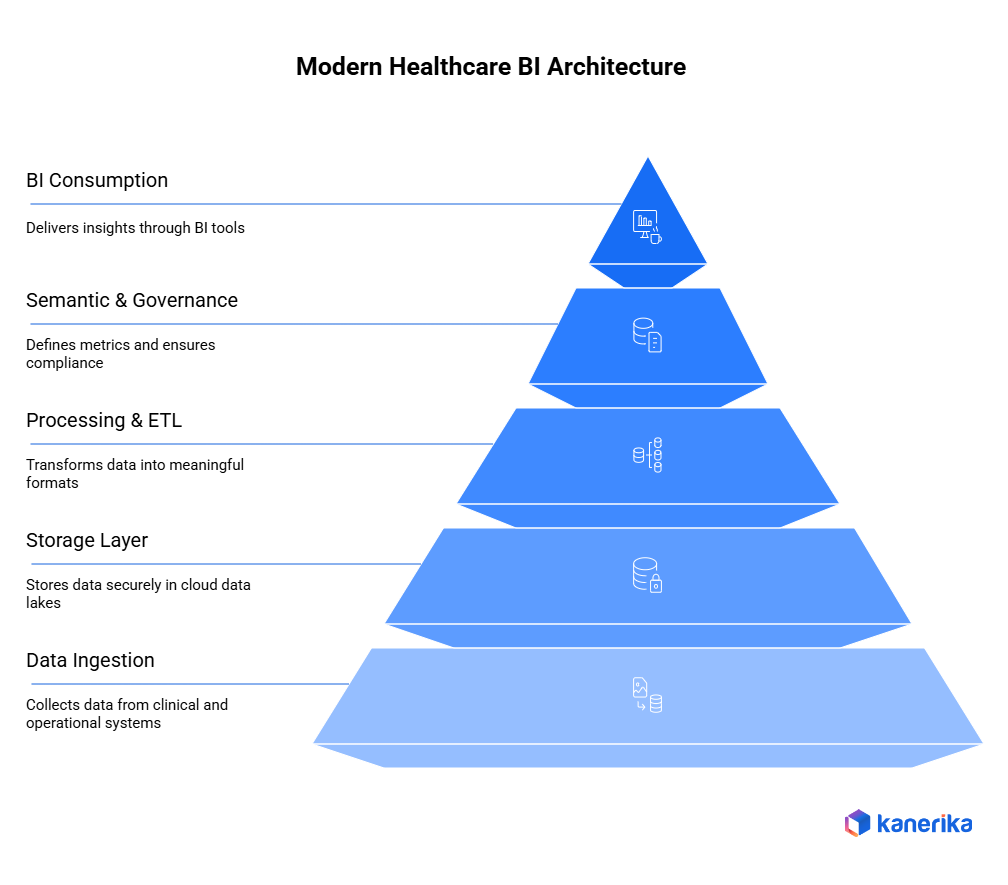
A modern healthcare BI stack is built in layers. Each layer has a specific function, and each must be designed with PHI handling, audit trails, and HIPAA compliance in mind from the start – not retrofitted after deployment.
1. Data Ingestion Layer
This layer pulls data from EHR systems (Epic, Cerner, Meditech), claims platforms, imaging archives, IoT devices, and operational systems. Modern ingestion uses event-driven pipelines with change data capture so updates flow in near real-time rather than nightly batch loads. HL7 FHIR standards govern how clinical data is structured and exchanged at this layer.
2. Storage Layer
Raw clinical and operational data lands in a cloud-native lakehouse – Azure Data Lake, AWS S3, or Google Cloud Storage – before being structured for query. The lakehouse model allows unstructured data (imaging, notes, audio) to coexist with structured data (lab results, billing codes) in a single governed environment.
3. Processing and ETL Layer
Transformation pipelines clean, standardize, and enrich incoming data. This is where ICD-10 codes are normalized, PHI is flagged and masked for non-clinical use cases, and clinical terminologies (SNOMED CT, LOINC) are mapped. Tools like Azure Data Factory, dbt, and FLIP handle orchestration at this layer.
4. Semantic and Governance Layer
The semantic layer sits between raw data and end-user consumption. It defines metrics, KPIs, and business rules so that “readmission rate” means the same thing in every dashboard across every department. Microsoft Purview and Unity Catalog are the leading tools for governance enforcement, managing who can access PHI, what they can see, and producing the audit logs HIPAA requires. Data integration at this layer determines whether clinical and operational teams get a consistent, trusted view of the organization.
5. BI Consumption Layer
The final layer delivers data to clinical and operational users through dashboards, self-service reports, and embedded analytics. Power BI, Tableau, and Looker are the primary tools here. Modern consumption layers also expose data via APIs for downstream clinical decision support systems.
Tools and Platforms for BI Migration in Healthcare
1. Modern BI Tools
Microsoft Power BI leads healthcare BI adoption among mid-market and enterprise health systems, primarily due to its native integration with Microsoft 365, Teams, and Azure. Row-level security and sensitivity labels make PHI handling more manageable than most competing platforms.
Tableau remains strong in academic medical centers and research hospitals where data exploration and custom visualization matter more than out-of-the-box integration.
Looker (Google Cloud) fits organizations already invested in BigQuery and Google Health Cloud infrastructure.
2. Cloud Data Platforms
Microsoft Fabric is the primary choice for organizations migrating off on-premise SQL Server, SSRS, or Azure Synapse. Its unified lakehouse architecture, native Power BI integration, and HIPAA-eligible services on Azure make it the natural landing zone for healthcare BI workloads in 2026.
Databricks is the preferred platform for analytics-heavy healthcare organizations – genomics research, population health modeling, and predictive clinical analytics at scale.
Snowflake fits multi-cloud environments where data needs to be shared across payers, providers, and partners without replication.
3. Healthcare Integration Tools
Azure Health Data Services provides a managed FHIR server that connects EHR data to the Azure data stack while maintaining HIPAA compliance. Mulesoft and Azure Integration Services handle HL7 v2, FHIR, and custom API connectivity between clinical systems and the data platform.
4. Governance Tools
Microsoft Purview covers data catalog, lineage tracking, sensitivity classification, and policy enforcement for PHI. Unity Catalog (Databricks) provides fine-grained access control and audit logging for Databricks-based healthcare stacks. Collibra handles enterprise data governance for large health systems managing multiple data domains.
5. Migration Accelerators
Migration accelerators reduce the manual effort of converting legacy reports, data models, and pipelines. Kanerika’s FLIP platform automates conversion of Crystal Reports, SSRS, Tableau, and Cognos dashboards to Power BI or Fabric – handling metadata migration, field mapping, and pipeline conversion in a structured workflow rather than a manual, report-by-report process. FLIP reduces migration effort by 50–60% and cuts timelines from months to 8–12 weeks for most healthcare environments.
| Category | Tool | Best Fit |
|---|---|---|
| BI Tools | Microsoft Power BI | Mid-market & enterprise health systems on Microsoft 365/Azure |
| Tableau | Academic medical centers, research hospitals | |
| Looker (Google Cloud) | Orgs on BigQuery + Google Health Cloud | |
| Cloud Data Platforms | Microsoft Fabric | Migrating off SQL Server, SSRS, Azure Synapse |
| Databricks | Genomics, population health, predictive clinical analytics | |
| Snowflake | Multi-cloud, cross-payer/provider data sharing | |
| Healthcare Integration | Azure Health Data Services | EHR-to-Azure via managed FHIR, HIPAA-compliant |
| MuleSoft / Azure Integration Services | HL7 v2, FHIR, custom API connectivity | |
| Governance | Microsoft Purview | PHI classification, lineage, policy enforcement |
| Unity Catalog (Databricks) | Fine-grained access control, audit logging | |
| Collibra | Large health systems, multi-domain governance | |
| Migration Accelerators | Kanerika FLIP | Crystal Reports, SSRS, Tableau, Cognos → Power BI/Fabric |
Step-by-Step BI Migration Roadmap for Healthcare
An effective BI migration within the healthcare sector needs to be well-organized, repeatable, and guard clinical information, maintain regulatory adherence, and enable real-time decision-making. The path ahead presents the critical actions that healthcare enterprises need to follow when transitioning over to new cloud-native and modern analytics systems that support their legacy BI systems.
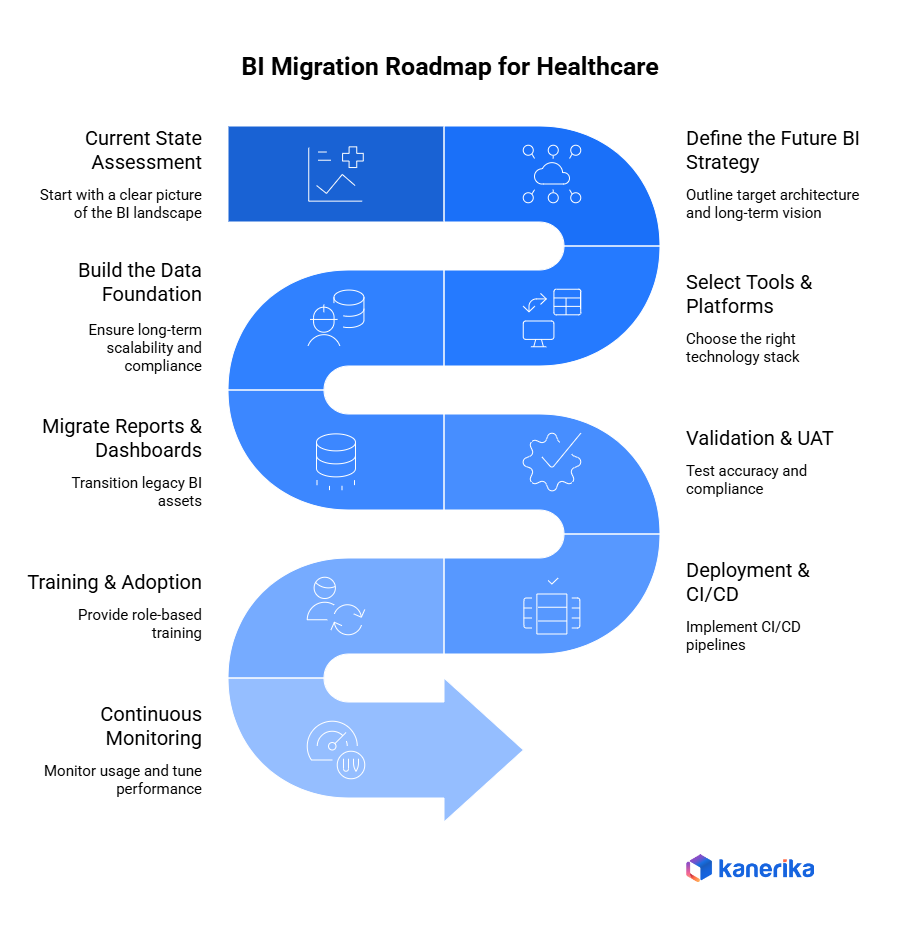
Step 1: Current State Assessment
It starts by having a clear picture of the current BI landscape.
- List all the reports, dashboards, OLAP cubes, scripts and data sources that are being used.
- Assess the data flow of EHR/EMR systems, PACS, LIS, RIS, billing, and claims management tools.
- Determine data silos which do not support the ability to do unified analytics.
- Review compliance gaps related to HIPAA, SOC 2, HITRUST, and internal audit requirements.
This assessment helps create a complete inventory and identifies high-risk areas.
Step 2: Define the Future BI Strategy
Next, healthcare organizations must outline their target architecture and long-term vision.
- Decide on a cloud-first, AI-ready BI architecture that supports predictive analytics and operational intelligence.
- Determine needs for real-time reporting, such as ER wait times, ICU capacity, bed occupancy, infection trends, and command-center visibility.
- Prioritize clinical, financial, and operational BI use cases to align the migration with organizational goals.
Step 3: Select Tools & Platforms
Choosing the right technology stack is a critical decision.
- Select the BI tool: Power BI, Tableau, or Looker, depending on governance, visualization, and embedded analytics needs.
- Choose the data platform: Databricks, Microsoft Fabric, Snowflake, or BigQuery to handle structured and unstructured clinical data securely.
- Define the governance model to support PHI protection, role-based access, lifecycle management, and lineage tracking.
Step 4: Build the Data Foundation
A strong foundation ensures long-term scalability and compliance.
- Ingest data using HL7/FHIR APIs, EHR interfaces, DICOM imaging transfers, and claims/insurance connectors.
- Build structured data layers: staging → curated → gold for clear separation of duties.
- Normalize clinical vocabulary using SNOMED, LOINC, ICD-10, CPT, and RxNorm to ensure consistency across reports.
Step 5: Migrate Reports & Dashboards
Once the foundation has been established, legacy BI assets are set back or reinvented.
- Use accelerators to map Tableau, Cognos, SSRS, or Qlik dashboards into modern BI tool equivalents.
- Redesign dashboards to fit clinical workflows for example, clinician summaries, patient flow visualizations, infection monitoring, or financial KPIs.
Step 6: Validation & UAT
There should be accuracy and compliance testing.
- Verify such clinical outcomes like LOS, readmission rates, the number of infections, and throughput.
- Test PHI/PII masking, row level security and access policies.
- Compare output to source EHR, billing, and financial systems to identify 100 percent integrity.
Step 7: Deployment & CI/CD
Once validated, the solution is ready for enterprise rollout.
- Implement CI/CD pipelines for BI artifacts.
- Publish certified datasets, semantic models, and governed metrics.
Step 8: Training & Adoption
User adoption determines long-term success.
- Provide role-based training for clinicians, administrators, finance teams, and operations managers.
- Run change-management workshops to ease the transition from legacy tools.
Step 9: Continuous Monitoring
Finally, continuous improvement keeps BI effective.
- Monitor usage analytics to identify valuable and underused reports.
- Tune performance for faster load times and optimized queries.
Best Practices for BI Migration in Healthcare
Migrating BI systems in the healthcare sector requires balancing clinical precision, regulatory requirements, and user adoption. The following seven practices define the difference between migrations that succeed and those that stall.
1. Prioritize Compliance and Patient Data Security
Because healthcare data contains highly sensitive PHI, compliance controls must lead every design and migration decision.
- Align BI architecture with HIPAA, HITECH, HITRUST, GDPR, and regional healthcare privacy standards.
- Implement PHI masking, tokenization, and differential privacy at the data layer, not the reporting layer.
- Enforce role-based access control so users access only the data their role requires.
- Maintain detailed audit logs for every access event and transformation. The HHS HIPAA Security Rule (hhs.gov/hipaa) specifies the technical safeguard requirements that BI architecture must address, including access controls, audit controls, and transmission security.
2. Build a Healthcare Semantic Layer
A unified semantic layer improves trust, consistency, and interoperability across clinical and operational reporting.
- Standardize definitions for core metrics: Length of Stay, mortality rate, average length of stay, OR utilization, and readmission rate.
- Create a clinical and financial glossary aligned with ICD-10, DRG, SNOMED, and CPT coding systems.
- Ensure all BI tools reference the same governed datasets so teams analyze consistent data regardless of the tool they use.
3. Use a Cloud-Native Foundation
Modern healthcare BI depends on scalable, compliant infrastructure.
- Use columnar storage formats like Parquet and governed lakehouse tables like Delta for both structured and unstructured data.
- Apply smart partitioning to support faster queries on PHI-heavy datasets such as claims, EHR events, and imaging metadata.
- Select platforms designed specifically for healthcare workloads – Databricks, Snowflake Healthcare Data Cloud, or Microsoft Fabric.
4. Adopt Metadata-Driven Pipelines
Metadata-driven approaches reduce manual work and support auditability across the full data lifecycle.
- Enable automated documentation during ingestion, transformation, and reporting stages.
- Use lineage tracking to map data journeys from EHR through the lakehouse to BI dashboards.
- Automate schema drift handling and validation to maintain long-term pipeline reliability as source systems change.
5. Focus on High-Value Dashboards First
To deliver early wins and support adoption, migrate the dashboards with the greatest operational and clinical impact first.
- Readmission dashboards that support risk scoring and targeted intervention programs
- Infection control dashboards for real-time surveillance and outbreak detection
- Patient flow dashboards covering ER wait times, ICU occupancy, and bed management
6. Implement a Strong Governance Framework
Governance ensures data accuracy, security, and consistent use across all reporting consumers.
- Form a centralized governance committee with representation from clinical, IT, and compliance leadership.
- Enforce automated policies for data retention and PHI masking.
- Certify datasets so end users can trust that what they are analyzing has been validated and approved.
7. Enable Self-Service BI for Clinicians and Managers
Giving healthcare teams access to safe, governed analytics directly increases BI adoption and reduces IT dependency.
- Provide pre-defined, governed datasets tailored to clinical, operational, and financial roles.
- Apply guardrails that prevent PHI exposure or unauthorized data combinations in self-service environments.
- Build data literacy through training and supported exploration so teams can answer their own questions without creating compliance risk.
Crystal Reports to Power BI Migration 2025: Key Considerations
Learn how to migrate from Crystal Reports to Power BI for modern, interactive analytics.
Real-World Case Studies
Healthcare organizations that have completed BI migrations report consistent improvements in reporting speed, data accessibility, and analytical capability.
1. Cleveland Clinic migrated its analytics infrastructure to Microsoft Azure to manage cross-departmental data at scale. Based on publicly reported outcomes, the migration improved data accessibility across clinical and research teams, enabled faster reporting cycles, and expanded the organization's capacity for outcomes-based research.
2. Kaiser Permanente moved its analytics services to cloud-based BI to handle the scale of its patient population and care network. Based on publicly reported outcomes, the platform now processes large-scale clinical data including EHR records, claims, pharmacy data, and population health metrics across its member base.
3. Mount Sinai Health System adopted the Databricks Lakehouse Platform to integrate clinical, operational, and research data in a unified environment. Based on publicly reported outcomes, the migration reduced data silos across the organization, accelerated research timelines, and improved decision-making for clinical leadership.
Future Trends in BI Migration for Healthcare
Healthcare analytics is moving from static dashboards toward AI-augmented, real-time intelligence. Cloud-native analytics adoption in large health systems has accelerated sharply over the past three years, driven by platform maturity, falling storage costs, and the availability of HIPAA-eligible managed services from all major cloud providers. The following eight trends define where healthcare BI is heading next.
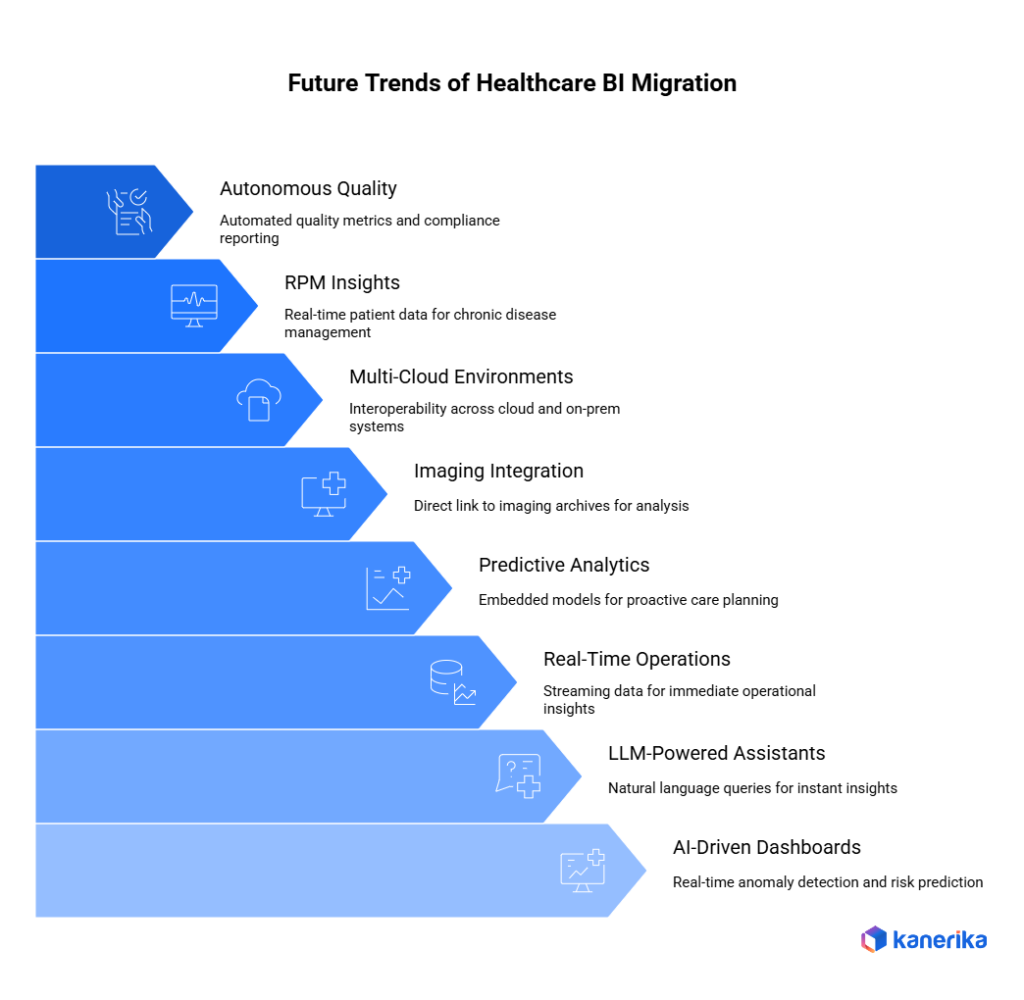
1. AI-Driven Clinical Dashboards
Healthcare BI is shifting from static reporting to AI-supported dashboards that surface anomalies, flag risks, and generate automated alerts before clinical teams need to search for them.
2. LLM-Powered BI Assistants for Clinicians
Large language models integrated into BI platforms will allow clinicians to ask natural-language questions – “Show sepsis risk for ICU patients today” – and receive governed, data-grounded answers without writing queries or navigating dashboards manually.
3. Real-Time Hospital Operations BI
BI systems will increasingly process streaming data from EHRs, IoT sensors, bed-tracking systems, and patient flow tools to deliver live operational dashboards that support same-day decisions.
4. Predictive Analytics Embedded in BI
Hospitals will embed predictive models for readmission risk, length of stay forecasting, infection spread, and staffing demand directly into dashboards, making predictive outputs available alongside historical metrics in the same view.
5. DICOM and Imaging Analytics Integration
Future BI environments will connect directly to imaging archives, making radiology throughput, scan volumes, and anomaly detection rates visible alongside clinical and operational metrics in unified dashboards.
6. Multi-Cloud BI Environments
Healthcare systems will implement multi-cloud strategies to meet regional data residency requirements, connect with payer and partner networks, and avoid vendor lock-in across their analytics infrastructure.
7. BI and Remote Patient Monitoring Integration
Remote patient monitoring devices will deliver real-time vital signs and device data that feed directly into BI dashboards, extending visibility from the hospital into home-based care settings.
8. Autonomous Quality-of-Care Dashboards
Agentic AI will automate the monitoring of quality metrics, detect deviations from clinical standards, and trigger review workflows automatically – reducing the manual effort required for ongoing quality assurance reporting.
Kanerika: Accelerating BI Migration for Healthcare Enterprises
Kanerika is an AI and data services company that helps healthcare organizations move off legacy reporting infrastructure without disrupting clinical operations or compliance posture. With certifications in ISO 27001 and SOC 2 Type II, and active partnerships with Microsoft and Snowflake, Kanerika works with mid-market and enterprise health systems navigating BI modernization across Power BI, Microsoft Fabric, and cloud data platforms.
For healthcare migrations specifically, Kanerika’s FLIP platform handles the conversion of Crystal Reports, SSRS, Tableau, and Cognos dashboards to Power BI or Microsoft Fabric – automating metadata migration, field mapping, and pipeline conversion in a structured workflow. Sensitivity labels and row-level security configurations carry forward into Power BI rather than being rebuilt manually per report, which matters when PHI is spread across hundreds of legacy assets.
In a recent engagement with a mid-sized health system, Kanerika completed an SSRS-to-Power BI migration covering 200+ clinical and operational reports in 10 weeks. Post-migration, the organization reduced reporting infrastructure costs by 40% and gained real-time visibility into patient throughput, bed utilization, and claims processing – metrics that previously required manual data pulls from three separate systems. Talk to Kanerika’s team to see how FLIP fits your environment.
Migrate to Power BI for Smarter Analytics and Real-Time Insights!
Partner with Kanerika for Seamless Migration Services.
Case Study: Fabric Migration for a Global Regulated Enterprise
The client, a renowned global participant in medical technology, is devoted to enhancing clinical decision-making, treatment pathways, and healthcare equipment management worldwide. With a dedication to innovation centered around patients, automation of workflows, and responsive customer service, they lead the way in medical technology advancement.
Challenges
- Disparate, siloed data sources and missing data mapping created inefficiencies and hindered decision-making
- Existing UI and UX design fell short of meeting the client’s expectations with a subpar healthcare dashboard, affecting user engagement and satisfaction
- The use of QlikView for data analysis with Power BI resulted in scattered reports in the healthcare dashboard and a time-consuming process, delaying critical insights
Solutions
- Leveraged Snowflake for centralized and global data mapping, eliminating silos and providing a unified view across verticals
- Implemented Power BI in this healthcare project with a user-friendly and intuitive UI/UX design, enabling data exploration and data-driven decisions
- Facilitated quick and comprehensive analysis via dashboards and reports, reducing the time to obtain valuable insights
Results
- 25% Increase in data-driven decisions
- 40% Decrease in response time
- 61% Reduction in time to information
Conclusion
Healthcare BI migration is no longer an infrastructure project – it is a clinical and operational priority. The organizations advancing fastest are those that treat the migration as a data strategy decision: choosing the right platform foundation, building the semantic layer before migrating reports, and governing PHI from the first pipeline stage rather than at the reporting edge. The technology is available and mature. The differentiator is execution discipline and the right implementation partner.
FAQs
What is BI migration in healthcare?
BI migration in healthcare is the process of moving business intelligence platforms, dashboards, reports, and data models from legacy systems to modern cloud-native environments while maintaining HIPAA compliance and data integrity throughout.
Why are healthcare organizations migrating their BI platforms?
Healthcare organizations migrate BI platforms to address limitations of legacy systems that cannot scale to current data volumes, meet modern compliance requirements, support real-time reporting, or integrate predictive analytics into clinical workflows.
What are the biggest challenges in healthcare BI migration?
The primary challenges include maintaining HIPAA compliance during data movement, preserving clinical data integrity across format transformations, managing complex EHR integrations, and driving adoption among clinical and administrative users.
How does healthcare BI migration ensure compliance and security?
Compliance is maintained through encrypted data transfers, role-based access controls, PHI masking at the data layer, detailed audit logging, and alignment with HIPAA, HITECH, and HITRUST frameworks throughout the migration process.
What data is typically included in healthcare BI migration?
Healthcare BI migration typically covers clinical data from electronic health records, financial data from billing and claims systems, imaging metadata, pharmacy records, operational data, and population health datasets.
How does BI migration improve patient care and operations?
BI migration improves patient care by enabling real-time clinical dashboards that surface actionable insights for clinicians, supporting predictive risk models, and giving operational leaders visibility into capacity, throughput, and quality metrics.
What should healthcare organizations look for in a BI migration partner?
Organizations should prioritize partners with demonstrated healthcare domain experience, HIPAA-compliant delivery processes, familiarity with EHR integration, proven migration accelerators, and certifications that reflect data security standards.
What is BI migration?
BI migration is the process of transferring business intelligence assets – reports, dashboards, data models, and semantic layers – from one platform or architecture to another, typically to gain scalability, compliance, or advanced analytics capabilities.









