Automate Claims Processing and Cut Operational Costs
Manual claims processing costs more than most carriers track. FLIP automates the entire lifecycle, so your team closes more files, catches leakage earlier, and never grows headcount to grow volume.
Reduced manual effort and delays
High Extraction Accuracy
Touchless Processing Rate
Faster Claims Processing Cycle
Reduction in Claims Leakage
Higher Customer Satisfaction
Get Started with Claims processing automation Solutions
What Insurers Lose with Manual Claims Processing?
Every manual step in claims adds cost, delays resolution, and creates room for fraud to go undetected.

Adjusters Spend Hours on Data Entry
Claims teams lose hours to document chasing and data entry across multiple disconnected systems.

Outdated Rules Lose to New Age Fraud
Rule-based fraud detection misses evolving schemes. Suspicious claims get paid and losses compound silently.

Claims Stall at Every Manual Handoff
Handoffs across adjusters, supervisors, and finance lack visibility. Approvals stall and cycle times balloon.
Where FLIP Transforms Insurance Claims Processing
FLIP automates document intake, validates claims against policy data, and routes approvals across teams. Adjusters spend less time on data entry and more on decisions.
Capture agent
Multi-Source Claims Capture
Pulls claims from policyholder portals, email, mobile uploads, EDI feeds, and SFTP. Every claim centralized automatically with deduplication and real-time tracking from first notice of loss.

Extraction agent
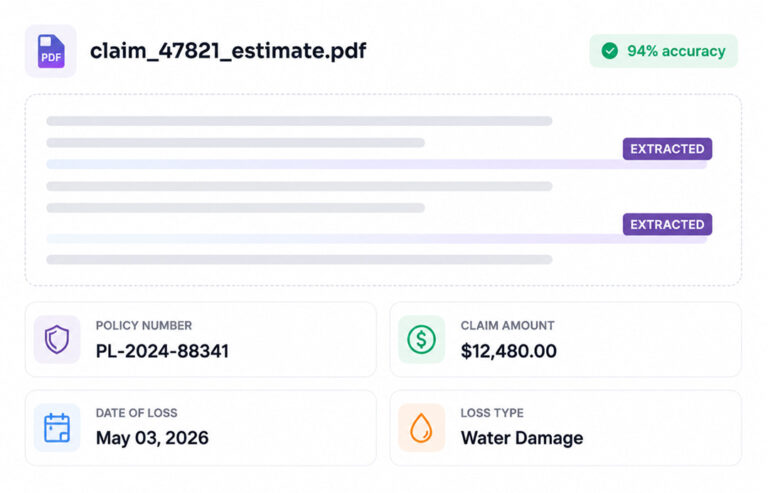
AI Document Extraction
Reads PDFs, scanned images, and email-body documents with high accuracy. Extracts policy details, damage estimates, and supporting evidence across formats without templates or manual indexing.
Matching agent
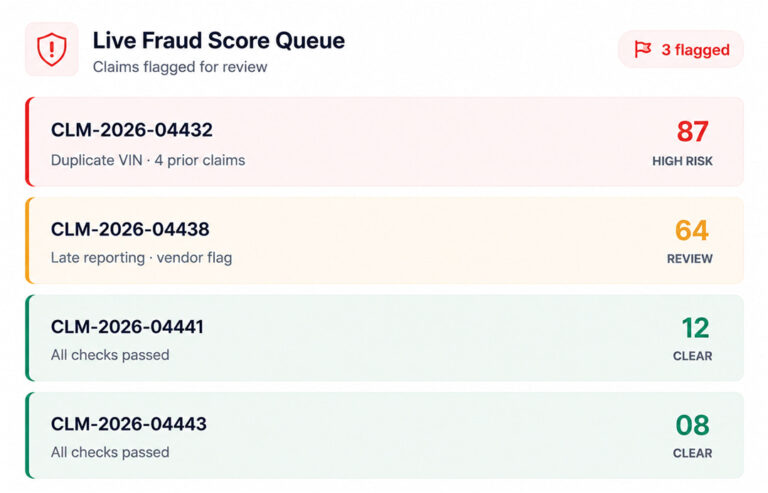
Intelligent Fraud Detection
Cross-references claim data against policy history and behavioral signals in real time. Flags duplicate submissions, inconsistencies, and high-risk patterns before a settlement decision is made.
Exception agent
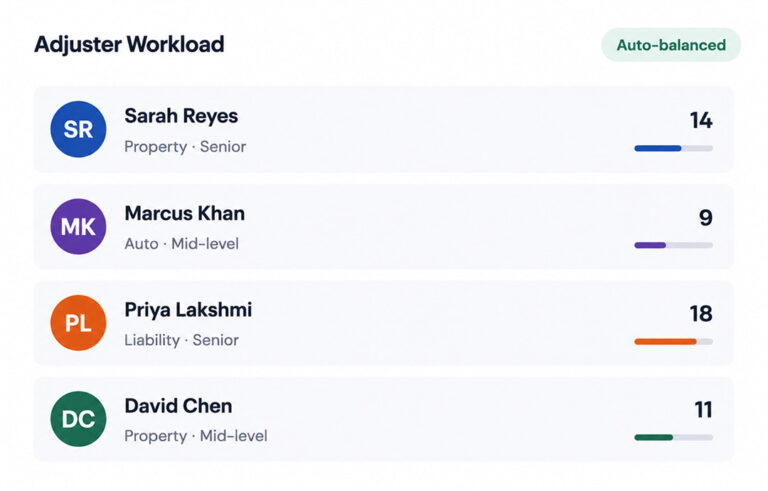
Smart Claims Routing
Routes claims to the right adjuster based on claim type, complexity, and workload. Escalation rules trigger automatically when SLAs are at risk, cutting assignment delays and inbox bottlenecks.
Posting & Governance
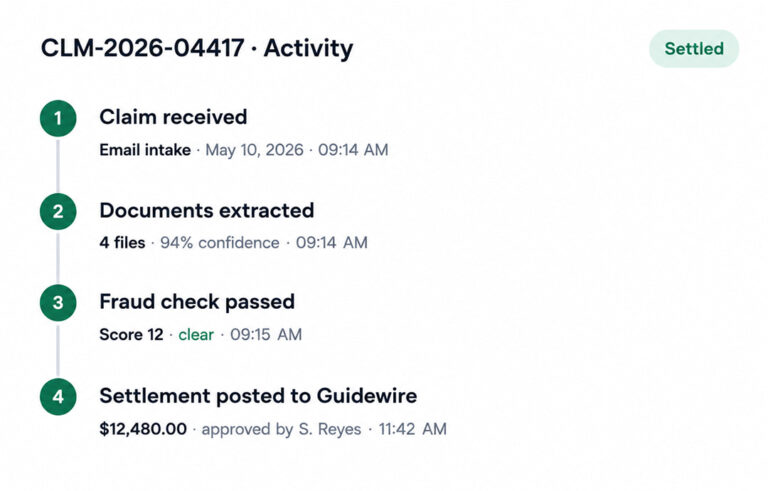
Settlement Posting and Audit Trail
Posts approved settlements directly to your core insurance system with pre-built connectors. Every action logged immutably for state regulatory, SOX, and internal audit requirements.
What Sets FLIP Apart from Legacy Claims Software
Most claims software automates steps. FLIP automates the entire lifecycle, with intelligence that adapts, integrates, and scales to how carriers actually operate.
Title
Others
FLIP
01
Intelligent Automation, Not Static Rules
Others
Rule-based fraud detection misses schemes that fall outside predefined patterns.
FLIP
Intelligent automation catches fraud patterns as they emerge.
02
Native Core System Connectivity
Others
Custom integrations with Guidewire and Duck Creek take months to build and maintain.
FLIP
Pre-built connectors for core insurance systems go live with no custom development.
03
Scales With Claims Volume
Others
Manual processes and legacy tools buckle when claim volumes spike unexpectedly.
FLIP
Automated claims processing handles higher volume without extra headcount
04
Compliance and Audit, Built In
Others
Audit trails require separate reporting tools and manual evidence pulls.
FLIP
Automatically logs every claim action for audit-ready compliance.
Who Benefits from FLIP Claims Automation
Claims automation only works when every role gets value from it. FLIP is built for the teams that run claims and the leaders who answer for them.
Loss Ratio Visibility
Real-time view of claims volume, cycle time, and leakage impact on the P&L
Full Operation Control
Monitor adjuster workload, exception rates, and SLA performance across every claim
Exceptions Only
Claims arrive with documents extracted, fraud scored, and context attached.
Evidence Available
Immutable, timestamped trail of every intake, fraud check, and settlement approval
Flexible Pricing Plans Tailored to Your Volume and Complexity
Every carrier runs claims differently. FLIP pricing adapts to your claim volume, core systems, and compliance requirements without forcing you into a fixed structure.
Pay-as-you-go
Volume-based
- Pay per claim processed.
- No minimum.
- Best for variable or seasonal claim volumes.
Monthly
- Unlimited volume.
- No lock-in and consistent operations
- Best for high-volume claims operations
Annual
- Dedicated CSM
- Enterprise SLA
- Volume pricing for multi-line rollouts
What Insurers Achieved with FLIP Claims Automation
Carriers across health, property, and liability have cut cycle time, reduced leakage, and scaled volume without growing their claims teams.
Eliminating Data Silos and Modernizing Analytics Infrastructure with Databricks
Impact:
- Zero Downtime, no production interruption
- 100% Legacy Infrastructure Decommissioned
- 100% Centralized governance, lineage, and data access
71% Higher Reporting Accuracy with Informatica to Databricks
Impact:
- 71% Higher Reporting Accuracy
- 38% Reduction in Data Handling Costs
- 64% Faster Decision-Making
80% Faster Document Processing with Databricks Workflows
Impact:
- 80% Faster Document Processing
- 95% Improved Metadata Accuracy
- 45% Accelerated Time-to-Insight
Common Questions About Claims Automation
01What is automated claims processing?
Automated claims processing uses software to handle the full insurance claims lifecycle without manual intervention. It covers intake, document extraction, fraud detection, adjuster routing, and settlement posting. Carriers that adopt automated claims processing reduce cycle time significantly, cut operational costs, and handle higher claim volumes without growing their teams. FLIP delivers end-to-end claims automation built for carrier-scale operations.
02What is claims leakage and how is it prevented?
Claims leakage refers to money paid out incorrectly through overpayments, duplicate settlements, missed subrogation opportunities, or fraud that slips through detection. Claims leakage prevention requires real-time validation at every stage of the lifecycle. FLIP cross-references claim data against policy history and behavioral signals continuously, flagging anomalies before settlements are approved rather than after payouts clear.
03What is the difference between claims processing software and traditional claims management systems?
Traditional claims management systems store and track claims but rely on manual steps for intake, validation, and routing. Modern claims processing software automates those steps end to end. The key difference is straight-through processing capability. Platforms like FLIP handle the full lifecycle automatically, from first notice of loss to settlement posting, while legacy systems still depend on adjusters to move claims through each stage.
04What claim types does FLIP support?
FLIP handles claims across auto, health, property, liability, and other lines of business within a single platform. It processes claims regardless of format, whether submitted through policyholder portals, email, mobile upload, EDI feeds, or SFTP. The same extraction and validation logic applies across claim types, so carriers do not need separate tools or configurations for different lines of business.
05How does intelligent document processing work for insurance claims?
Most carriers reach production with FLIP within three to four weeks. Deployment includes a parallel run against the existing claims process so teams can validate accuracy and build confidence before full cutover. Pre-built core system connectors remove the lengthy integration work that makes legacy claims automation projects take quarters. The result is faster time to value without the risk of a big-bang implementation.
06How does insurance claims automation software work?
Insurance claims automation software captures claims from multiple sources, extracts data from supporting documents, validates against policy records, and routes exceptions to the right adjuster automatically. Advanced claims processing software like FLIP goes further by applying intelligent fraud detection and posting approved settlements directly to core insurance systems, creating a fully connected and auditable claims lifecycle.
07 How does intelligent document processing work for insurance claims?
Intelligent document processing for insurance claims uses OCR combined with language models to extract structured data from PDFs, scanned images, and email documents without templates. It handles police reports, medical records, repair estimates, and multi-document claim files with high accuracy. Unlike template-based tools, it adapts to new document formats automatically, removing the manual indexing that slows every claims operation down.
08Can insurance fraud detection be fully automated?
FLIP comes with pre-built connectors for major core insurance platforms including Guidewire and Duck Creek, as well as banking and ERP systems. Integrations go live in weeks without custom development. Every connection supports real-time data sync, eliminating overnight batch processing. Carriers keep their existing systems in place while FLIP handles the automation layer across the full claims lifecycle.
08How does FLIP handle claims exceptions and escalations?
When FLIP identifies a claim that requires human review, it routes the exception automatically to the right adjuster based on claim type, complexity, jurisdiction, and current workload. Each exception arrives with full context attached, extracted documents, fraud score, policy data, and a recommended next action. Escalation rules trigger automatically when SLAs are at risk, ensuring no claim sits unattended without a reason.



