Mayo Clinic faced a challenge that would make any healthcare executive lose sleep. In January 2025, they expanded their AI documentation partnership with Abridge to serve 2,000 clinicians treating around a million patients. But here’s what makes this remarkable: they’re doing it while maintaining some of the strictest data governance standards in healthcare.
Mayo Clinic has built internal accountability systems for safe, effective, and ethical implementation of artificial intelligence in medical practice. Their approach demonstrates how robust governance frameworks enable innovation rather than blocking it. When data governance works properly, organizations can pursue cutting-edge technologies without compromising patient safety or regulatory compliance.
This transformation didn’t happen overnight. Mayo Clinic’s Center for Individualized Medicine underwent digital transformation to equip clinicians with tools to analyze data and unlock critical insights for patient care. The result? Enhanced diagnoses, improved treatments, and better patient outcomes across their entire health system.
Healthcare organizations today manage exponentially more data than ever before. Healthcare data alone is projected to reach 10,000 exabytes by 2025. Without proper governance, this massive volume becomes a liability rather than an asset.
Ready to transform your healthcare organization’s data strategy like Mayo Clinic?
Schedule a consultation to explore governance solutions tailored to your specific needs.
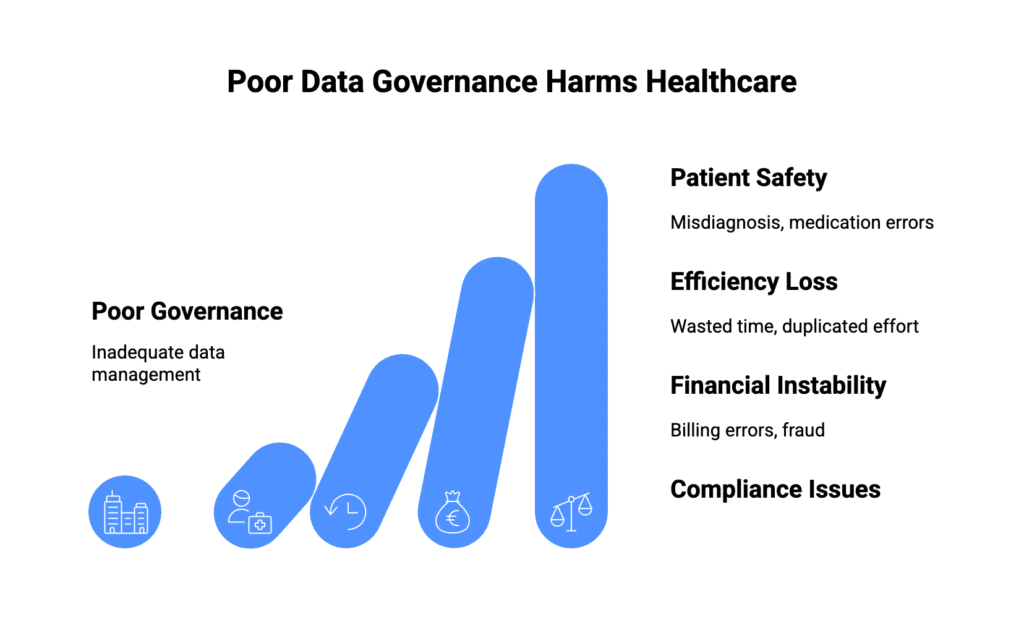
The Real Cost of Poor Healthcare Data Governance
VillageCareMAX discovered this truth the hard way. Before implementing proper governance, their healthcare plan struggled with data integrity issues that undermined decision-making confidence. Duplicate patient records created billing confusion. Incomplete medical histories frustrated physicians. Outdated information led to inappropriate care recommendations.
The numbers tell a sobering story about industry-wide governance failures. Provider directories are inaccurate 49 percent of the time according to Centers for Medicare and Medicaid Services data. When patients get referred to out-of-network specialists unnecessarily, everyone loses. Patients face higher costs and delayed care. Healthcare systems lose revenue and patient trust.
But the real cost isn’t financial. It’s human.
Consider what happens when a patient arrives at an emergency department with chest pain. Without proper data governance, the attending physician might not have access to the patient’s complete cardiac history. Previous EKGs remain trapped in a cardiology system. Medication lists sit incomplete in a primary care database. Lab results from last month never integrated properly.
The physician makes treatment decisions based on incomplete information. That’s not clinical incompetence—that’s governance failure.
How Effective Governance Transforms Patient Care
Organizations that implement comprehensive governance frameworks don’t just avoid problems—they create competitive advantages that directly benefit patients.
Clinical Decision Support Revolution
Strong governance enables physicians to make better decisions faster. When patient data flows smoothly between systems, clinical decision support tools can provide real-time alerts about drug interactions, allergy conflicts, and evidence-based treatment recommendations.
Michelle Hoiseth, Chief Data Officer of Parexel, explained how proper governance helps leverage data from electronic medical record systems, claim systems, and pharmacy claims systems to see the impact of new treatments. This comprehensive view transforms research capabilities and patient care quality simultaneously.
“…as we move into leveraging new sources of data, it’s on us to be able to look any patient in the eye and say, ‘We’ve done the best job we can here. We stand behind this result and the analysis, and that’s us all coming to the table together.’”
- Michelle Hoiseth, Chief Data Officer of Parexel
Consider a diabetic patient visiting multiple specialists. With proper governance, the endocrinologist sees recent lab values from primary care. The cardiologist accesses blood pressure trends from home monitoring devices. The ophthalmologist reviews previous retinal screening results. Each specialist makes informed decisions based on complete information rather than isolated snapshots.
Population Health Management Excellence
Governance frameworks enable population health initiatives that identify at-risk patients before they require expensive interventions. Organizations can analyze patterns across large patient populations to predict which individuals need preventive care, medication adjustments, or lifestyle interventions.
These capabilities proved invaluable during COVID-19. The World Economic Forum highlighted that accurate and trustworthy data helped with disease control tasks, including predicting illness spread, identifying infection clusters, and tracking carrier contacts. Organizations with strong governance responded more effectively to the pandemic while maintaining routine care quality.
Operational Efficiency Gains
Healthcare margins remain tight, making efficiency improvements essential for sustainability. A hospital that centralizes its data management can reduce costs associated with managing multiple fragmented systems, freeing up resources for patient care.
The math works beautifully. Through referential and probabilistic modeling methods, a repository with data from 7 million patients could be trimmed to 1 million patient records. Organizations reduce storage costs, improve system performance, and eliminate the administrative overhead of managing duplicate information.
Staff productivity improvements provide measurable benefits. When nurses can quickly access complete medication histories, they spend more time with patients and less time searching through multiple systems. When physicians receive automated alerts about critical lab values, they respond faster to urgent situations.
Ready to transform your healthcare organization’s data strategy?
Schedule a consultation to explore governance solutions tailored to your specific needs.
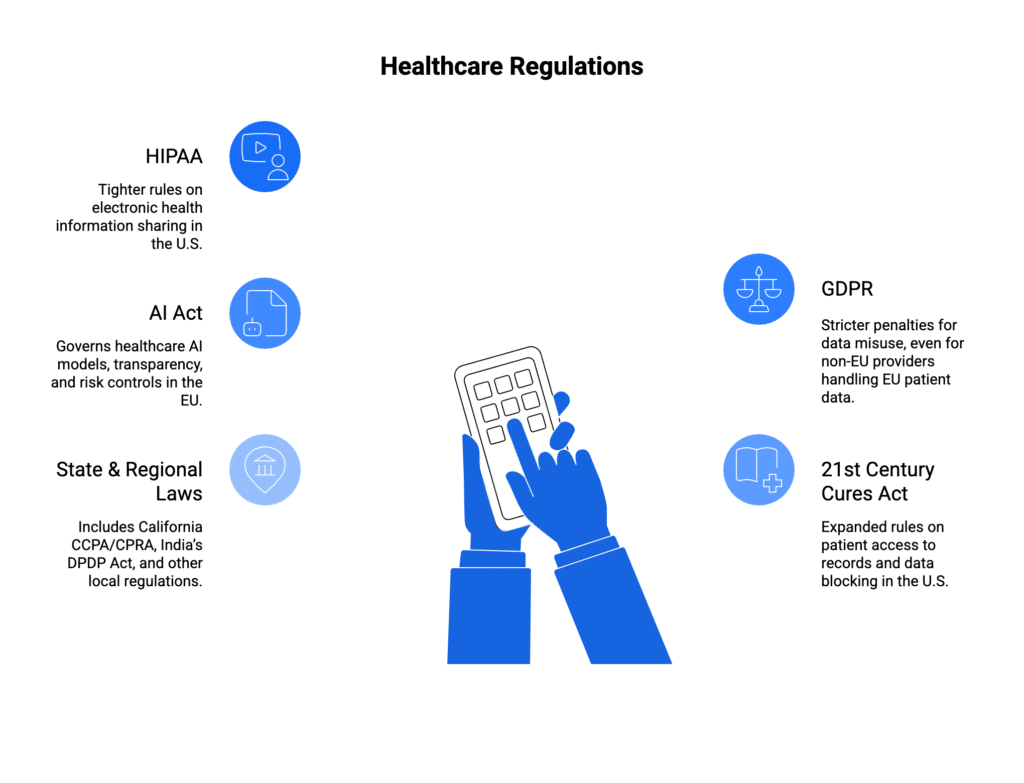
Navigating the 2025 Regulatory Environment
Healthcare data governance operates within an increasingly complex regulatory framework. Recent changes require immediate attention from compliance teams and technology leaders alike.
HIPAA Security Rule Revolution
The HHS Office for Civil Rights proposed the first major update to the HIPAA Security Rule in 20 years on January 6, 2025. This update specifically addresses AI integration challenges that didn’t exist when the original rule was written.
The new requirements focus on several critical areas that organizations must address immediately:
Organizations using AI systems that process protected health information must implement documented security and privacy controls. Regular AI audit procedures become mandatory for healthcare providers. Algorithmic bias testing and mitigation protocols must be established before AI deployment.
Enhanced third-party vendor oversight requirements apply to all AI systems accessing patient data. Organizations can no longer treat AI vendors differently from traditional business associates.
These changes reflect regulatory recognition that AI represents both tremendous opportunity and significant risk in healthcare settings. Organizations that proactively address these requirements will have competitive advantages over those scrambling to achieve compliance.
State-Level AI Regulation Complexity
2025 brings new state laws on AI regulation with varying privacy protections across different healthcare contexts. Organizations operating across multiple states face complex compliance matrices that require sophisticated governance approaches.
Some states focus on algorithmic transparency requirements. Others emphasize bias testing and patient notification obligations. Still others mandate specific security controls for AI systems processing health information. The patchwork creates challenges that centralized governance frameworks must address systematically.
Multi-state healthcare systems need governance policies that meet the most stringent requirements across all jurisdictions while maintaining operational efficiency. This often means implementing controls that exceed minimum requirements in some states to ensure consistent compliance everywhere.
International Compliance Considerations
The General Data Protection Regulation affects healthcare organizations serving EU citizens, regardless of where the organization is located. French authorities fined Dedalus Biologie, a medical software company, 1.5 million euros in 2021 for GDPR non-compliance due to inadequate security measures.
Healthcare organizations with international patients or research collaborations must integrate GDPR requirements into their governance frameworks. This includes explicit consent mechanisms, data portability rights, and strict breach notification procedures that don’t interfere with clinical workflows.
Microsoft Fabric Adoption: A Practical Guide for Enterprises
Cut through the noise—learn how to adopt Microsoft Fabric with practical steps that actually work for enterprises.
Essential Technical Capabilities to Ensure Data Governance in Healthcare
Building effective governance requires specific technical and operational capabilities. Organizations need more than good intentions and policy documents to manage healthcare data effectively.
Intelligent Data Discovery and Cataloging
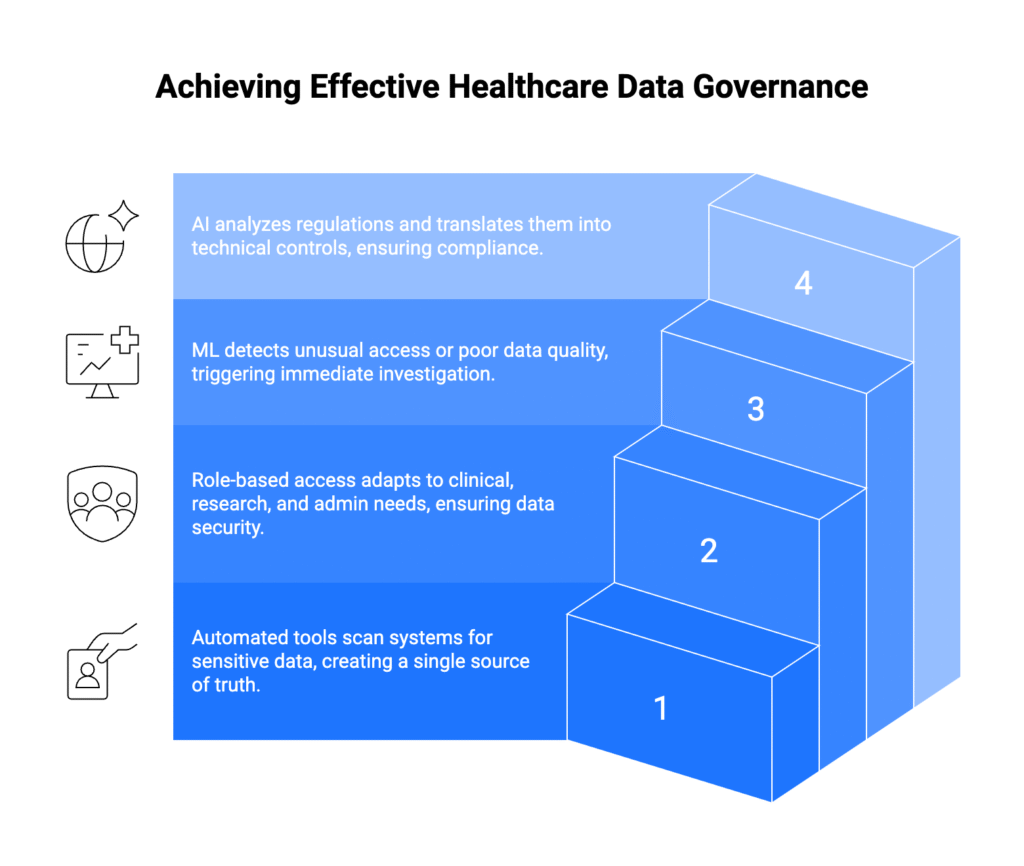
Modern healthcare organizations generate data faster than humans can catalog it manually. Automated discovery tools identify sensitive information across all organizational systems, creating comprehensive inventories that support both compliance and clinical operations.
An enterprise data catalog acts as the central nervous system for healthcare data governance. When a physician searches for a patient’s cardiac history, the catalog instantly surfaces relevant records from cardiology visits, emergency department encounters, and routine primary care appointments.
Automated metadata harvesting ensures catalogs remain current as systems change and data grows. Machine learning algorithms classify new data types and suggest appropriate governance controls based on sensitivity levels and usage patterns.
Advanced Access Control Systems
Healthcare requires more sophisticated access controls than traditional business environments. Emergency situations demand immediate data access for patient safety. Research applications need de-identified datasets. Billing departments require financial information without clinical details.
Role-based access control systems adapt to these complex requirements. Emergency department physicians can access complete patient records during critical situations. Research staff receive only de-identified data sets appropriate for their studies. Administrative staff see billing information without accessing clinical notes.
Automated access reviews prevent former employees from retaining system permissions. Time-based access controls ensure temporary staff receive appropriate permissions that expire automatically. Audit logs track every data interaction for compliance documentation.
Real-Time Monitoring and Incident Response
2024 saw a spike of interest in third-party risk management as security events dominated headlines. Healthcare organizations need governance frameworks that detect and respond to threats immediately rather than discovering problems during annual audits.
Modern monitoring systems use machine learning to identify unusual access patterns, potential data quality issues, and security threats. When a staff member attempts to access an unusually large number of patient records, the system flags the activity for review. When data quality metrics fall below established thresholds, relevant teams receive immediate notifications.
Real-time incident response capabilities prevent small issues from becoming major compliance violations or security breaches. Automated escalation procedures ensure appropriate stakeholders receive notifications based on incident severity and organizational protocols.
AI-Powered Policy Management
Artificial intelligence streamlines governance policy creation by analyzing existing organizational data, suggesting appropriate controls, and automating policy updates as regulations change. These capabilities become increasingly valuable as organizations manage larger datasets and more complex compliance requirements.
Natural language processing helps organizations parse regulatory documents and translate legal requirements into actionable technical controls. Machine learning algorithms automatically classify new data types and recommend governance policies based on similar existing datasets.
However, AI governance tools must themselves comply with healthcare regulations. Organizations need verification that AI systems processing patient data meet updated HIPAA requirements and undergo regular bias testing to prevent discriminatory outcomes.
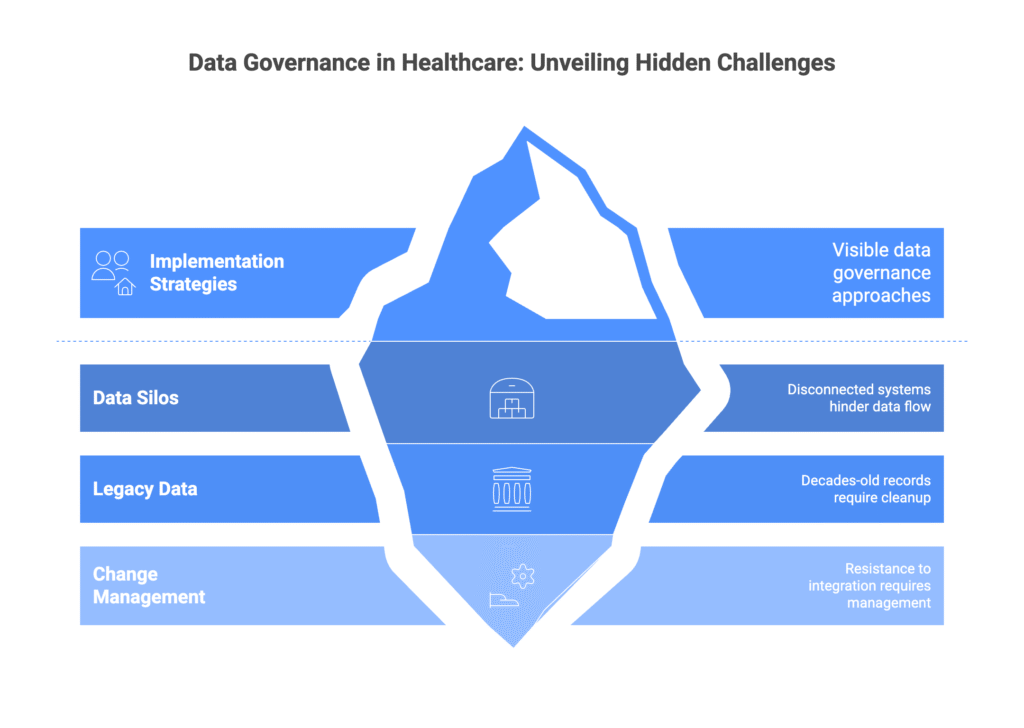
Implementation Strategies That Deliver Results
Healthcare organizations typically fall into three categories when approaching governance implementation. Understanding which category applies helps determine the most effective implementation strategy.
The Foundation Builders
Some organizations start from scratch and need comprehensive frameworks. These organizations benefit from proven implementation methodologies that establish governance incrementally rather than attempting massive transformation overnight.
Shannon refers to a “one-time cleanup” as a common starting point for organizations improving their data repositories. This strategic preparation addresses decades of accumulated data inconsistencies before implementing new governance controls.
Through systematic cleanup processes, organizations often reduce their data footprint dramatically while improving quality. Duplicate records disappear. Incomplete information gets completed or removed. Outdated records from deceased patients are archived appropriately.
The Silo Breakers
Other organizations have basic governance structures but struggle with data silos across on-premises and cloud environments. These organizations need integration strategies that unite disparate systems without disrupting ongoing operations.
The challenge intensifies when clinical systems, administrative platforms, and research databases operate independently. Patient information exists in multiple places with different formats, quality standards, and access controls.
Successful silo integration requires careful planning and phased execution. Organizations must maintain system functionality while gradually implementing unified governance policies. Change management becomes critical as staff adapt to new workflows and data access procedures.
The Innovation Enablers
Advanced organizations want to scale existing governance for new applications like AI analytics and population health management. These organizations seek to become “enterprise-ready and future-proof” their governance investments.
Innovation enablers focus on emerging technologies that require high-quality, well-governed data. AI-powered clinical decision support, predictive analytics, and personalized medicine initiatives depend on comprehensive governance frameworks that ensure data reliability and regulatory compliance.
How to Choose the Right Technology for Healthcare Data Governance
Selecting the right technology for healthcare data governance is not just about features; it’s about finding a solution that ensures compliance, protects patient data, and supports everyday operations.
- Regulatory compliance – Ensure the technology supports HIPAA, GDPR, or other local healthcare regulations.
- Data security – Look for encryption, role-based access controls, and audit trails.
- Interoperability – The system should integrate with EHRs and other healthcare platforms.
- Scalability – Choose tools that can handle growing volumes of patient data.
- Ease of use – Staff adoption depends on intuitive design and simple workflows.
- Vendor support – Check for regular updates, responsive support, and training.
- Reporting and monitoring – Strong analytics and oversight features improve data governance.
Kanerika is a recognized leader in data governance solutions, enabling healthcare organizations to unlock better patient care through secure, accurate, and accessible data management systems. By partnering with Kanerika, hospitals and healthtech providers benefit from tailored frameworks, proven technologies, and real-world impact across operational, clinical, and compliance needs.
Kanerika’s Approach in Healthcare
Kanerika’s methodology centers on unifying fragmented records, establishing centralized data catalogs, and implementing cloud-based platforms for robust governance. Their layered approach spans data quality, security, interoperability, and compliance to meet HIPAA, GDPR, and local regulations. Leveraging tools such as Microsoft Purview, PowerBI, and automation frameworks, Kanerika empowers organizations with actionable insights, ensuring every patient’s information is managed with integrity and confidentiality.
Case Studies: Kanerika in Action
A global healthcare provider struggling with siloed systems partnered with Kanerika to revamp their architecture. By implementing cloud technologies and advanced governance, they streamlined data processing, improved patient self-care tools, and increased operational agility. The outcome included substantial reductions in response times and errors, with enhanced scalability for evolving medical needs.
A healthtech leader dealing with fragmented device tracking and operational inefficiencies adopted Kanerika’s Power BI-powered solution. The result was sharper insights, lower costs, and elevated patient safety through real-time analytics and seamless data integration.
In another case, Kanerika addressed poor data quality and inconsistent classification at a hospital by introducing a centralized data catalog. This not only cut report generation time by 45% but also boosted decision-making and data accessibility by over 90% and 70%, respectively.
Measurable Patient Care Benefits
Kanerika’s data governance solutions deliver:
- A unified patient record that provides clinicians a holistic view for informed treatments.
- Error reduction by ensuring data consistency and reliability across systems.
- Streamlined communication and collaboration for patients needing coordinated care between specialties.
- Real-time dashboarding and predictive analytics for proactive, personalized patient interventions.
Why Kanerika?
Partnering with Kanerika means leveraging deep expertise in data management, analytics, and automation. Their tailored governance frameworks help healthcare institutions strengthen compliance, maximize care quality, and foster innovation in an era of accelerating digital transformation. Kanerika’s commitment to ongoing support, staff training, and technology adoption ensures a sustainable, future-ready patient data ecosystem.
AI in Robotics: Pushing Boundaries and Creating New Possibilities
Explore how AI in robotics is creating new possibilities, enhancing efficiency, and driving innovation across sectors.
Frequently Asked Questions
What is the role of data governance in healthcare?
Data governance in healthcare establishes the policies, procedures, and accountability frameworks that ensure patient information remains accurate, secure, and accessible to authorized personnel. It defines who owns healthcare data, how it flows between systems, and what compliance standards must be met under regulations like HIPAA. Effective healthcare data management reduces clinical errors, enables interoperability across EHR systems, and supports population health analytics. Without governance, hospitals risk data breaches, regulatory penalties, and compromised care quality. Kanerika helps healthcare organizations implement robust data governance frameworks that balance security with clinical accessibility—schedule a consultation to assess your current state.
Why is data governance important in healthcare?
Data governance is critical in healthcare because it protects sensitive patient information while ensuring clinical teams can access accurate data for treatment decisions. Healthcare organizations handle vast amounts of protected health information across disparate systems, making standardized governance essential for HIPAA compliance and meaningful use requirements. Strong data governance reduces duplicate records, improves care coordination, and enables reliable analytics for population health initiatives. It also minimizes legal exposure from data breaches that can cost millions in penalties and reputational damage. Kanerika’s data governance solutions help healthcare providers build compliant, efficient data ecosystems—reach out for a tailored assessment.
Why is data governance important in hospitals?
Hospitals require data governance to manage complex data flows across emergency departments, labs, pharmacies, and patient records while maintaining regulatory compliance. Hospital data governance ensures consistent patient identifiers across systems, reducing medical errors caused by duplicate or mismatched records. It establishes clear ownership for clinical and operational data, enabling faster decision-making during critical care situations. Governance frameworks also support hospital accreditation requirements and payer reporting obligations. Without proper controls, hospitals face increased readmission rates, billing errors, and audit failures. Kanerika partners with hospital systems to implement governance frameworks that improve data quality and clinical outcomes—contact us to explore solutions.
How does data governance improve patient care?
Data governance improves patient care by ensuring clinicians access complete, accurate, and timely health information at the point of care. When governance frameworks standardize data definitions and enforce quality controls, providers can trust the information in EHR systems for diagnosis and treatment planning. Clean patient data enables personalized medicine, reduces adverse drug interactions through accurate medication histories, and supports care coordination across specialists. Governance also facilitates predictive analytics that identify at-risk patients before conditions worsen. Better data quality directly correlates with improved clinical outcomes and patient satisfaction scores. Kanerika helps healthcare providers connect data governance to measurable patient care improvements—let’s discuss your priorities.
What are the 5 pillars of data governance?
The five pillars of data governance are data quality, data management, data policies, data stewardship, and data security. Data quality ensures accuracy and completeness across systems. Data management addresses storage, integration, and lifecycle processes. Data policies define standards, access rules, and compliance requirements. Data stewardship assigns accountability for data domains to specific roles. Data security protects against unauthorized access and breaches. In healthcare, these pillars work together to maintain patient data integrity while meeting HIPAA and other regulatory mandates. Each pillar requires dedicated resources and executive sponsorship to succeed. Kanerika builds comprehensive data governance programs around these pillars—connect with our team to strengthen your foundation.
What are the 4 pillars of data governance?
The four pillars of data governance are data quality, data security, data compliance, and data management. Data quality focuses on accuracy, consistency, and completeness across all sources. Data security establishes access controls, encryption, and breach prevention measures. Data compliance ensures adherence to regulations like HIPAA, GDPR, and industry standards. Data management covers the technical infrastructure for storage, integration, and data lifecycle processes. Healthcare organizations must balance all four pillars to protect patient information while enabling clinical and operational analytics. Weak governance in any pillar creates enterprise-wide risk exposure. Kanerika designs governance frameworks that address all four pillars cohesively—request a free governance maturity assessment today.
What is an example of data governance?
A practical data governance example in healthcare is implementing a master patient index with standardized data quality rules. This governance initiative assigns data stewards to oversee patient identity management, establishes matching algorithms to prevent duplicate records, and creates policies for merging or correcting errors. The governance framework defines who can access patient identifiers, how changes are audited, and what compliance documentation is required. This single initiative improves clinical safety, billing accuracy, and regulatory compliance simultaneously. Healthcare organizations often start governance programs with high-impact use cases like this before expanding scope. Kanerika helps clients identify and execute governance quick wins—talk to us about starting your program.
What are the four main roles in data governance?
The four main data governance roles are data owner, data steward, data custodian, and data governance council member. Data owners are senior leaders accountable for data domains within their business areas. Data stewards manage day-to-day data quality, definitions, and policy enforcement. Data custodians handle technical implementation, including storage, security, and access provisioning. Governance council members set enterprise strategy, resolve cross-functional conflicts, and approve policies. In healthcare settings, clinical and IT leadership must collaborate across these roles to balance patient care needs with compliance requirements. Clear role definitions prevent accountability gaps that lead to data issues. Kanerika helps organizations define and operationalize these governance roles effectively—schedule a workshop with our experts.
What are the 3 key elements of good data governance?
The three key elements of good data governance are people, processes, and technology. People includes establishing clear roles like data stewards and owners with defined accountability. Processes encompasses the policies, standards, and workflows that govern data throughout its lifecycle. Technology provides the platforms for data cataloging, quality monitoring, lineage tracking, and access control. Healthcare organizations often over-invest in technology while neglecting the people and process foundations that make tools effective. Successful governance programs balance all three elements with executive sponsorship and measurable objectives tied to clinical and business outcomes. Kanerika takes a balanced approach to governance implementation across all three elements—connect with us to evaluate your readiness.
What are the five areas of data governance?
The five areas of data governance are data quality management, metadata management, data security and privacy, data architecture, and data lifecycle management. Data quality management ensures accuracy and consistency across systems. Metadata management catalogs data assets with business definitions and lineage. Data security and privacy controls access and protects sensitive information. Data architecture establishes standards for integration and interoperability. Data lifecycle management governs data from creation through archival or deletion. Healthcare organizations must address all five areas to meet regulatory requirements and enable trusted analytics for population health and clinical decision support. Kanerika delivers governance solutions spanning all five areas—reach out for a comprehensive roadmap tailored to healthcare.
What are the eight major goals of data governance?
The eight major data governance goals are improving data quality, ensuring regulatory compliance, reducing data-related risks, enabling data-driven decisions, establishing accountability, increasing operational efficiency, supporting data security, and maximizing data value. Healthcare organizations prioritize compliance and quality goals to meet HIPAA requirements and clinical safety standards. Risk reduction addresses breach prevention and audit readiness. Decision enablement supports population health analytics and care optimization. Accountability clarifies ownership across clinical and administrative domains. Efficiency goals reduce redundant data management efforts. These goals must align with organizational strategy and include measurable KPIs for tracking progress. Kanerika helps healthcare clients define and achieve governance goals with proven frameworks—let’s build your roadmap together.
What are the four key functional areas of data governance?
The four key functional areas of data governance are data quality, data operations, data compliance, and data architecture. Data quality functions define standards, monitor metrics, and remediate issues. Data operations manage daily processes for integration, transformation, and delivery. Data compliance ensures adherence to regulations like HIPAA and handles audit documentation. Data architecture establishes technical standards for data models, storage, and interoperability. Healthcare organizations need all four functional areas working together to support clinical workflows, research initiatives, and regulatory reporting. Gaps in any area create downstream problems affecting patient care and operational efficiency. Kanerika structures governance programs around these functional areas for measurable impact—contact us to optimize your data operations.
What are the first four phases of data governance?
The first four phases of data governance are assessment, planning, implementation, and operationalization. Assessment evaluates current data maturity, identifies pain points, and inventories existing data assets. Planning defines governance vision, roles, policies, and prioritized initiatives with executive sponsorship. Implementation deploys governance tools, establishes data steward networks, and executes initial use cases. Operationalization embeds governance into daily workflows with monitoring, metrics, and continuous improvement processes. Healthcare organizations should complete assessment thoroughly before rushing to technology purchases. Each phase builds foundations for sustainable governance that adapts as regulations and organizational needs evolve. Kanerika guides healthcare clients through all governance phases with proven methodologies—start with our assessment services.
What are the 7 pillars of clinical governance?
The seven pillars of clinical governance are clinical effectiveness, risk management, patient experience, communication effectiveness, resource effectiveness, strategic effectiveness, and learning effectiveness. Clinical effectiveness ensures evidence-based care delivery. Risk management identifies and mitigates patient safety threats. Patient experience focuses on satisfaction and engagement. Communication effectiveness enables information flow across care teams. Resource effectiveness optimizes staff and equipment utilization. Strategic effectiveness aligns clinical activities with organizational goals. Learning effectiveness promotes continuous education and improvement. Data governance supports all seven pillars by ensuring accurate, accessible information for clinical decisions and quality reporting. Kanerika helps healthcare organizations leverage data governance to strengthen clinical governance outcomes—explore our healthcare solutions today.